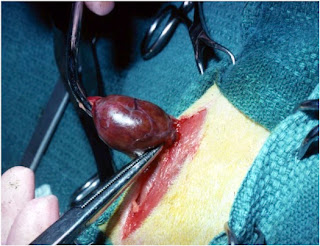
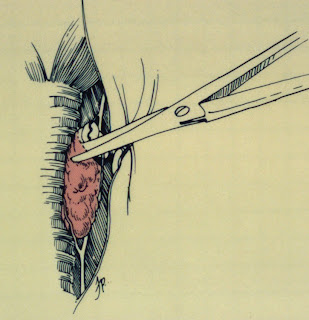
One major disadvantage of selecting surgical thyroidectomy as the treatment used for a cat with hyperthyroidism is that sedation and anesthesia must be given in order to complete the operation (1-3). Cats with hyperthyroidism are generally older and commonly have concurrent or multisystemic disease, which can increase anesthetic risk (4-6).
Although the mortality rate is very low, morbidity due to anesthesia, which is often overlooked, is not uncommon. Provided that the potential risk is recognized, suitable premedication, a smooth anesthetic induction, careful monitoring, appropriate attention to the oxygenation, ventilation and circulation will ensure a very low morbidity rate in cats.
In this post, I will review suggested protocols for sedating and anesthetizing cats with hyperthyroidism.
Considerations for Preanesthetic Management
Cats with hyperthyroidism are generally older and may suffer from a concurrent disease, in addition to the damage caused by the high circulating thyroid hormone concentrations.
The most significant risk pertaining to anesthesia results from cardiac changes in hyperthyroid patients. In addition to a rapid heart rate (tachycardia), cardiac murmur, and a gallop rhythm, many of these cats develop thickening of the left ventricle, predisposing them to myocardial hypoxia, arrhythmias, and cardiac arrest (3-5).
 If possible, it is always recommended that we use antithyroid drugs (e.g., methimazole or carbimazole) to treat the hyperthyroid cat medically for a few weeks before surgery in order to render the cats euthyroid before anesthesia. For more information, see my previous post on Preoperative Preparation of the hyperthyroid cat.
If possible, it is always recommended that we use antithyroid drugs (e.g., methimazole or carbimazole) to treat the hyperthyroid cat medically for a few weeks before surgery in order to render the cats euthyroid before anesthesia. For more information, see my previous post on Preoperative Preparation of the hyperthyroid cat.Preanesthetic Preparation
An overnight fast is required to help ensure that the a cat will have an empty stomach. Water need not be deprived until premedication is given or until about 2 hours prior to anesthesia.
On the day in which anesthesia and surgery is planned, the veterinarians should conduct a thorough physical examination, including auscultation for cardiac arrhythmias and murmurs. If concurrent kidney or liver disease is suspected, repeat laboratory testing should be done and intravenous fluid therapy administered if needed.
An IV catheterization is placed, generally in either the cephalic and saphenous veins. Use of SC premedication is generally recommended prior to placement of the IV line in these cats.
Premedication (Preanesthetic Agents)
Even very friendly cats often object to physical restraint, sometimes making the anesthetic induction procedure extremely difficult to accomplish safely. Therefore, use of preanesthetic sedation is recommended in order to facilitate IV catheter placement and anesthetic induction in these hyperthyroid cats (3-5). This sedative also has an anesthetic-sparing effect during the maintenance anesthetic period.
 In hyperthyroid cats, use of an opioid agent administered subcutaneously is suggested for its cardiovascular safety and analgesia (5-9). Such opioid drugs commonly used include hydromorphone (0.025-0.05 mg/kg), oxymorphone (0.025-0.05 mg/kg), or methadone (0.3-0.5 mg/kg). These opioid agents help create a sense of well-being or euphoria, but they do not typically sedate cats very well. Therefore, it is best to combine one of these opioid agents with another drug to produce the desired sedative effect.
In hyperthyroid cats, use of an opioid agent administered subcutaneously is suggested for its cardiovascular safety and analgesia (5-9). Such opioid drugs commonly used include hydromorphone (0.025-0.05 mg/kg), oxymorphone (0.025-0.05 mg/kg), or methadone (0.3-0.5 mg/kg). These opioid agents help create a sense of well-being or euphoria, but they do not typically sedate cats very well. Therefore, it is best to combine one of these opioid agents with another drug to produce the desired sedative effect.Combining an opiate drug either with a mild tranquilizer or sedative is commonly done in veterinary practice. The benzadiazepine tranquilizers (diazepam or midazolam) cause only minimal cardiovascular depression and are therefore very useful preanesthetic agents for hyperthyroid cats (5,6,9,10). The dissociative agent ketamine, is a useful preanesthetic agent. However, this drug can produce an increased heart rate, cardiac output, and blood pressure and should never be used alone, especially if administered intravenously or at high doses (1,4).
A number of drug protocols are available for premedication prior to induction (3,4,5,7). Combinations of an opioid (e.g., hydromorphone, oxymorphone, or methadone) administered with a tranquilizer (e.g., midazolam [Versed]) is one commonly used protocol. Alternatively, use of a dissociative agent (e.g., ketamine [Ketaset]) given with a mild tranquilizer (midazolam) is also a popular choice among veterinarians.
As an alternative, a combination of 3 agents — a subcutaneous opioid (see doses above), midazolam (0.1-0.2 mg//kg, SC), and very low-dose ketamine (2 mg/kg, SC) — can be used to sedate fractious cats (5).
Such drug combinations also provide better restraint and analgesia than that achieved by single drug administration and have fewer side effects than the use of one class of preanesthetic alone. For example, when used alone, opioids can induce extreme excitement or “mania,” ketamine will produce increased severe muscle rigidity and excessive salivation, and midazolam may induce paradoxical excitement and dysphoria. When combined with other CNS depressants, these side effects will occur less frequency and are much milder.
Anesthesia Induction
Placement of electrocardiogram (ECG) and Doppler equipment prior to induction of anesthesia is ideal. The ECG detects rhythm abnormalities, and Doppler assesses blood pressure changes and provides an audible pulse signal during this critical time.
Again, a number of protocols can be used for induction of anesthesia in cats with hyperthyroidism. One protocol that is very safe for the cardiovascular system entails the intravenous administration of both etomidate (0.5–1.5 mg/kg) and a benzodiazepine (eg, diazepam or midazolam, 0.1–0.3 mg/kg). However, etomidate has the potential to cause adrenal suppression and lower serum cortisol levels, warranting supplementation with physiological doses of glucocorticoids in some cats.
Alternatively, slow IV administration of propofol (2-6 mg/kg) provides rapid induction but should be used judiciously, as this agent can produce vasodilation and hypotension. Respiratory arrest is not uncommon, particularly with rapid IV bolus. The drug is best given slowly and titrated to effect in order to produce an anesthetic level just deep enough to allow endotracheal intubation.
Maintenance Anesthesia (Inhalation Agents)
Endotracheal intubation and use of an inhaled anesthetic agent is recommended. A number of inhaled anesthetic agents are available but isoflurane or sevoflurane, are most commonly employed (1,3).
The advantages of inhalation anesthesia in cats with hyperthyroidism include the following: a patent airway, rapid control of anesthetic depth, and quick and smooth recovery (11). Disadvantages of these anesthetic agents include a degree of cardiovascular depression (e.g., myocardial depression, hypotension, and slowing of the heart). An IV infusion of an opioid drug (e.g., fentanyl 5–10 μg/kg/hr) can be used concurrently to facilitate reduction in the inhaled agent dose and to improve cardiovascular performance (5).
Anesthetic Support and Monitoring
Anesthetic monitoring is important to maintain a proper plane of anesthesia and to prevent excessive insult to the cardiovascular, respiratory, and central nervous systems.
Heart rate, rhythm, and blood pressure should be monitored during surgery. Hyperthyroid cats are prone to a number of arrhythmias (e.g., premature ventricular contractions, supraventricular tachycardia), as well as hyper- and hypotension. If arrhythmias develop in hyperthyroid in cats during anesthesia, treatment with a short-acting beta-blocker, such as esmolol (50 μg/kg/min) is recommended (4-6). Alternatively, small doses of IV propranolol (a longer-acting beta-blocker) may be carefully administered (1).
A balanced electrolyte solution should be administered IV with goal of maintaining cardiac filling without overloading the heart. In hyperthyroid cats with concurrent kidney disease, the fluids should be administered before and during anesthesia, and continued during the recovery period.
Body temperature should be monitored in all cats undergoing general anesthesia. Because of the tendency for anesthetized cats to lose body heat, supplemental heat sources are often required to maintain adequate body temperature (100-103.5 ̊F).
Recovery
A quiet, stress-free environment is ideal. Fluids should be continued in patients with renal compromise and analgesics provided as needed. Oxygen should be provided at least until extubation of the cat but may be helpful until full recovery.
Body temperature must be maintained so as not to prolong the recovery, and lessen oxygen requirement by muscle tissues. Forced warm air blankets or circulating warm water blankets are very effective in maintaining the body temperature, but warmed fluid bags or infra-red lamps are also useful external heat sources.
Bottom Line
Many choices are available to tailor anesthetic protocols to meet the demand of the hyperthyroid cat. A smooth induction of anesthesia, careful monitoring in oxygenation, circulation and ventilation, and close attention to fluid balance and smooth recovery, all are important steps in ensuring a safe anesthetic protocol for the hyperthyroid cat.
References:
- Peterson ME: Considerations and complications in anesthesia with pathophysiologic changes in the endocrine system. In: Short CE (ed), Principles and Practice of Veterinary Anesthesiology. Philadelphia, Williams and Wilkins Co. 1987;251-270.
- Peterson ME, Randolph JF, Mooney CT: Endocrine diseases, In: Sherding RG (ed): The Cat: Diagnosis and Clinical Management (2nd Ed) New York, Churchill Livingstone. 1994;1404-1506.
- Panciera DL, Peterson ME, Birchard, SJ: Diseases of the thyroid gland. In: Birchard SJ, Sherding RG (eds): Manual of Small Animal Practice (Third Ed), Philadelphia, Saunders Elsevier, pp 327-342, 2006.
- Jacobson JD. Sedating and anesthetizing patients that have organ dysfunction. Vet Med 2005;100:518-526.
- Mama K. Anesthesia for thyroid gland disease. Clinician's Brief 2012;July:37-40.
- Keon TP, Templeton JJ. Diseases of the endocrine system. In Katz J, Steward DJ (eds): Anesthesia and Uncommon Pediatric Diseases. WB Saunders, Philadelphia. 1987;311-344.
- Bateman SW, Haldane S, Stephens JA. Comparison of the analgesic efficacy of hydromorphone and oxymorphone in dogs and cats: a randomized blinded study. Vet Anaesth Analg 2008;35:341–347.
- Pascoe PJ. Opioid analgesics. Vet Clin North Am Small Anim Pract. 2000;30:757-72.
- Schaafsma IA, Pollak YW, Barthez PY. Effect of four sedative and anesthetic protocols on quantitative thyroid scintigraphy in euthyroid cats. Am J Vet Res 2006;67:1362-1366.
- Nordt SP, Clark RF. Midazolam: a review of therapeutic uses and toxicity. J Emerg Med 1997;15:357-65.
- Clarke KW. Options for inhalation anaesthesia. In Practice 2008;30: 513–518.